Top government health chief declares 'long COVID' doesn't really exist, study finds flu impairs more people in the long term

A new study has found that the post-viral effects of COVID-19 are no worse than other respiratory illnesses, such as the flu. The study's author – a top government health official in Australia's state of Queensland – declared that it is time to retire the "long COVID" term because it is harmful and misleading.
Dr. John Gerrard is Queensland's Chief Health Officer, a leading infectious disease specialist, and previously was the Director of Infectious Diseases at the Gold Coast Hospital.
Gerrard is also the lead author of a recent study that found the post-viral effects of COVID-19 to be equal to or even less severe than other respiratory illnesses.
"We believe it is time to stop using terms like 'long Covid.' They wrongly imply there is something unique and exceptional about longer-term symptoms associated with this virus," Gerrard proclaimed. "This terminology can cause unnecessary fear, and in some cases, hypervigilance to longer symptoms that can impede recovery."
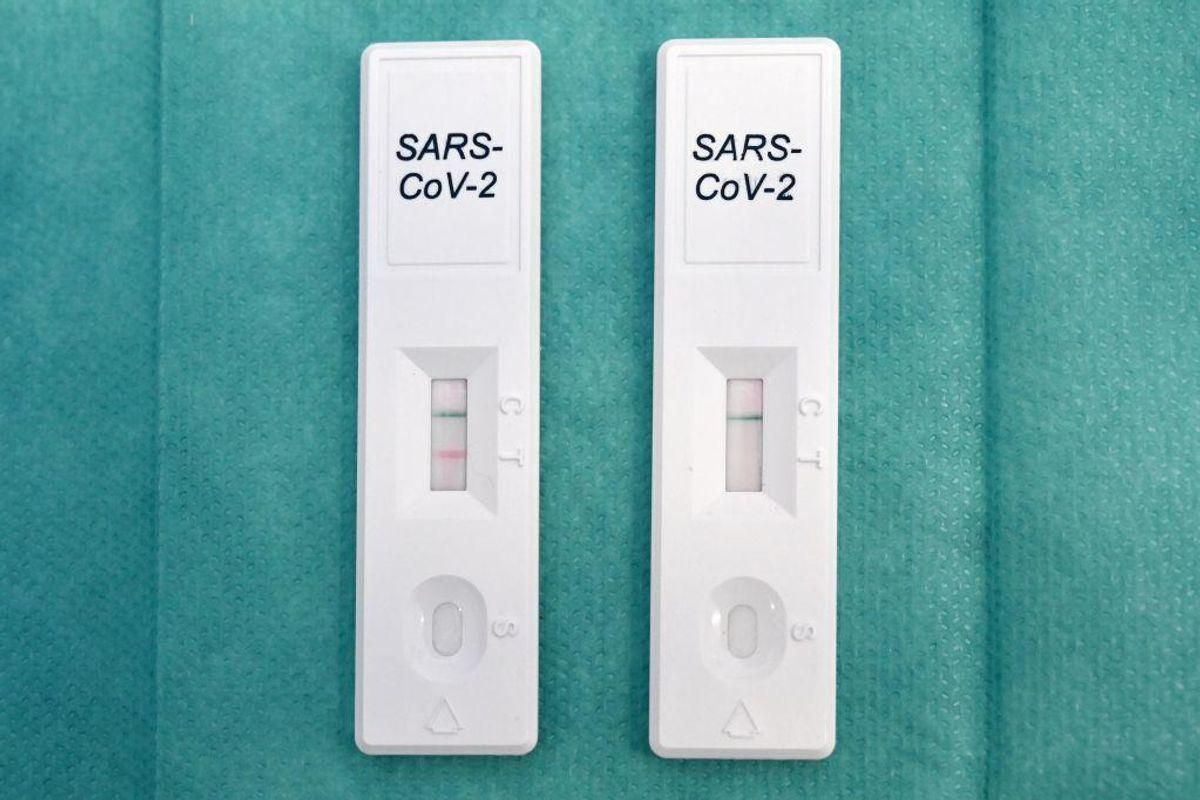
The study examined 5,112 adults who had symptoms of a respiratory illness and underwent PCR testing between May and June 2022. Of those individuals, 2,399 tested positive for COVID-19, while 995 tested positive for influenza, and 1,718 tested negative for both.
A year after their PCR tests, the participants in the study were asked about ongoing symptoms.
Of the respondents, 16% said they felt ongoing symptoms a year later, and 3.6% reported moderate-to-severe impairment.
In fact, the people who were infected with the flu had a higher rate of impairments a year later, according to the study.
According to the progressive outlet The Guardian, "The 3% of the study participants who had ongoing impairments after COVID-19 infection was similar to the 3.4% with ongoing impairments after influenza."
The Australian Broadcasting Corporation reported, "Dr. Gerrard said 94 percent of participants who reported the moderate to severe level of functional limitations experienced fatigue, post-exertion symptom exacerbation, brain fog and changes to taste and smell a year after their infection."
Gerrard will present the study next month at the European Congress of Clinical Microbiology and Infectious Diseases in Barcelona.
"Our evidence suggests that there isn't, that it is not dissimilar to other viruses," Gerrard declared. "That does not mean that you can't get these persistent symptoms following COVID-19, but you're no more likely to get it after COVID than with other respiratory viruses."
Gerrard emphasized, "But in the vast majority of people, recovery is the norm."
Gerrard said during a Friday press conference, "I want to make it clear that the symptoms that some patients described after having COVID-19 are real, and we believe they are real. What we are saying is that the incidence of these symptoms is no greater in COVID-19 than it is with other respiratory viruses, and that to use this term 'long COVID' is misleading and I believe harmful."
Like Blaze News? Bypass the censors, sign up for our newsletters, and get stories like this direct to your inbox. Sign up here!